
Osteoporosis, Osteopenia, Bone Loss and Menopause: The Hormone Solution for Stronger Bones
Osteoporosis, Osteopenia, Bone Loss and Menopause: The Hormone Solution for Stronger Bones
When you’re going through menopause, your body is going through a lot of changes. You may be dealing with frustrating symptoms like hot flashes, weight gain, and mood swings—and those are enough to make you want to scream.
However, there are some symptoms of menopausal hormone decline that you may not be able to see or feel, but can be life-threatening: osteoporosis, or thinning bones.
Osteoporosis affects more than 25 million people in the United States—and it’s more common than you might think.
Are You Worried About Your Bone Health?
Osteoporosis is responsible for about 1.5 million fractures in the U.S. every year. In fact, one in two women over the age of 50 will break a bone due to osteoporosis (compared to 1 in 4 men), and that’s not even counting the people who’ve already broken a bone but don’t know it yet.

If this sounds scary, that’s because it is. Every year 300,000 hip fractures occur and 20 percent of those impacted die within a year, while half never regain their independence.
In fact, more U.S. women die each year from complications from hip fractures than from breast cancer. Sixty percent of women over the age of 50 have either osteoporosis or low bone mass (osteopenia).
To state that a bit differently, the statistics are pretty shocking. Once a woman reaches age 65, if she has a fall there is a 50% chance that she will lose mobility for life. And 20% of those women will die within the year.
Most women don’t even realize they have bone loss until they break something or their doctor orders a bone density test—which means that by the time you’re diagnosed with osteoporosis or low bone mass (osteopenia), you could already have been living with these conditions for years without even knowing it.
We know it’s not fun to think about, but osteoporosis is a serious disease. It is a silent disease that can lead to debilitating fractures and long-term disability.
That’s why it’s important to start taking care of yourself now so you can avoid any potential issues down the road. After all, thinning bones don’t happen overnight—and they won’t develop overnight either.
What is Osteoporosis, exactly?
Osteoporosis is a condition in which the bones lose mass and density, making them fragile and more likely to break. The bone tissue in people with osteoporosis is less dense and weaker than that of people without the disease. This makes it easier for bones to break or fracture when they’re put under stress or subjected to an impact like falling or bumping into something.
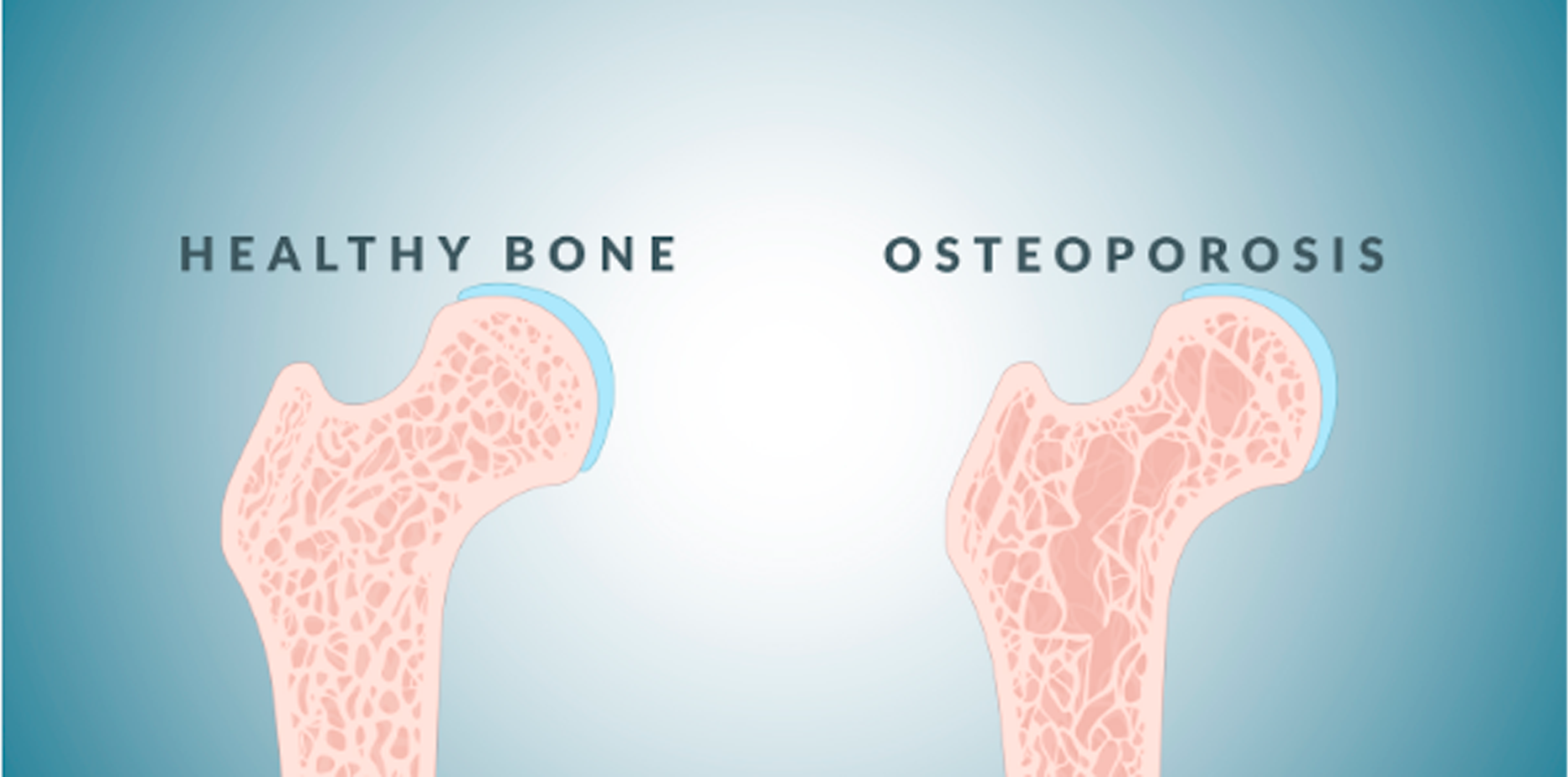
Osteoporosis can also cause changes in your posture and balance, making you more likely to fall and break a bone.
It’s most common in older women and it can make everyday tasks like getting out of bed or climbing stairs difficult. So, if you’re going through menopause, you’re at an even greater risk of developing osteoporosis than other women are! The number one reason for bone loss is estrogen loss. And we will all lose estrogen as we enter perimenopause and menopause. Progesterone and testosterone are also contributors to bone health, just to a lesser degree.
The good news? If caught early enough and treated properly, osteoporosis is treatable and even reversible.
That’s why it’s important to understand how menopause affects your bone health, and what you can do about it.
Causes of Osteoporosis

It’s not just a matter of getting old—it’s about losing calcium from our bones faster than it can be replaced by our bodies. So what causes this imbalance?
While genetics play a role, other factors include lack of exercise, hormonal changes during menopause, genetics, age, lifestyle factors such as diet and exercise, and medications.
The Bone Connection: Menopause and Osteoporosis

It’s no secret that women are at a greater risk for osteoporosis than men, but many people aren’t aware of the connection between osteoporosis and menopause. For women, the most common cause of osteoporosis is menopause.
Here’s why: The primary cause of osteoporosis is a decrease in estrogen, which occurs naturally during menopause.
So, why do people lose bone density?
Osteoporosis occurs when your body’s rate of bone breakdown outpaces the rate of new bone formation.
As we age, our bodies produce less and less estrogen, which is necessary for strong bones. Estrogen helps to build strong bones and keep them healthy by increasing bone density and slowing down bone loss as you age.
When estrogen levels fall, the bones become less dense. This happens because bone tissue is constantly being replaced with new bone tissue through a process called remodeling. To put it simply, when estrogen levels drop, your body can’t produce new bone tissue at the same pace that it breaks down old tissue. The result is a loss of bone density over time, which means bones become weaker and more likely to break. This can lead to osteoporosis.
Estrogen also helps maintain strong bones by increasing the amount of calcium your body absorbs from food, and it also increases the amount of calcium stored in your bones.
This is why women are more likely than men to develop osteoporosis (though men can also get it).
How Your Hormones Affect Your Bone Health
You may think that the strength of your bones and muscles is based solely on genetics, but it’s actually hormones that control the health of your bones, cartilage, tendons, and ligaments.
When you’re young, it’s easy to think that your bones and joints will always be strong—as long as you exercise. But the reality is that over time, your body produces fewer sex hormones, causing the cartilage and tendons in your joints to weaken. That’s why many athletes experience injuries they didn’t when they were younger.
Hormones play a huge role in the strength and flexibility of not only your bones but also your muscles, cartilage, tendons, and ligaments.
They are dependent on all three sex hormones—estrogen, progesterone, and testosterone—without which your bones become brittle and weak. Without adequate levels of these sex hormones, your bone and cartilage weaken.
Tendons need adequate estrogen; without enough estrogen in your body, tendons become stiffer and less flexible—this increases the risk for injury because less flexible tendons can’t absorb shock as they would otherwise.
Ligaments also require estrogen; without enough estrogen in your body, ligaments become brittle and weak—this increases the risk of ligamentous injury by making them more susceptible to tearing or rupture.
In order to maintain lean muscle mass as you age, you need adequate testosterone. Testosterone plays a huge role in maintaining lean muscle mass, which tends to decline with age as well.
And the amount of testosterone left after menopause depends on whether your body has enough DHEA to convert into testosterone.
When these hormones decline past a certain point during perimenopause and menopause, it can become more difficult to maintain lean muscle mass and strength…and it isn’t just about every individual hormone–it’s about having hormone balance.
Secondary Causes of Osteoporosis

There are several other factors that can contribute to osteoporosis besides loss of estrogen:
Behaviors: Certain behaviors can increase your risk for osteoporosis, including smoking, excessive alcohol consumption, poor diet, and lack of exercise. Smoking causes your bones to lose calcium faster than normal; heavy drinking may also increase your risk for developing osteoporosis because it interferes with the absorption of nutrients including calcium–both of which are necessary for healthy bones.
Conditions – These conditions include celiac disease or kidney disease that affects the absorption of nutrients from food. Conditions such as hyperthyroidism (a thyroid disorder), rheumatoid arthritis (an autoimmune disease), and vitamin D deficiency can also increase your risk of developing osteoporosis.
Diseases – Diseases like cancer or lupus may impact bone health.
Disorders – Disorders like kidney failure or diabetes can affect the production of hormones needed to build strong bones. And medications like steroids or chemotherapy can also have an impact on bone health.
Osteoporosis: Risk Factors and Symptoms

Osteoporosis can be a scary diagnosis, but it’s not one to panic over.
While osteoporosis can affect anyone, there are some risk factors that increase the likelihood of developing this condition. Some of these include:
Age: As you get older, your bones become less dense and more likely to fracture or break.
Gender: Women—especially post-menopausal women—are at the highest risk for osteoporosis.
Family History: If you have a parent who has been diagnosed with osteoporosis or has experienced multiple fractures due to bone breaks (which is common among seniors), then there’s an increased chance that you’ll also develop this condition. However, it is important to not let your family history define you. The actions you take today can change your outcomes and break the cycle.
Bone Structure and Body Weight: People who have narrow hips and small frames tend to have a higher risk of osteoporosis because their bones are not as strong as those who have wider hips or larger builds.
Race/Ethnicity: Whites are more likely than African Americans or Hispanics to develop osteoporosis. Asians may also be at increased risk for this condition compared with other races/ethnicities—but we don’t know enough about this topic yet!
People Who Have Had Weight-Bearing Fractures in the Past Year (examples include wrist or hip fractures)
While it’s true that your family history and other risk factors can increase your chances of developing osteoporosis, even if you think you don’t have any risk factors, you could still be at risk for this disease. In fact, many people who develop osteoporosis aren’t aware of any risk factors at all!
If you do have osteoporosis, though, here are some of the possible symptoms:
-Loss of height (weakening of the vertebrae)
-Back pain or pain in the hips or lower back
-Stooped posture
-Fractures (broken bones) that don’t heal properly
-Inability to perform normal activities due to pain or discomfort (e.g. difficulty getting up after sitting or lying down)
If you are experiencing any of these symptoms, it’s important to get a bone density scan (DEXA) as soon as you can.
The Conventional Treatment for Osteoporosis
If you’re diagnosed with osteoporosis, you may be offered treatments that can slow down or stop further bone loss. Conventional treatment for osteoporosis focuses on managing symptoms and preventing new fractures.
The conventional treatment for osteoporosis is medication. The most common form of medication prescribed is a bisphosphonate (e.g., Actonel®, Boniva®, Reclast®), and teriparatide (Forteo®). This drug works by slowing down bone loss by reducing the activity of cells in the bone. It also helps to maintain adequate blood calcium levels. Prolia is another medication that works in a similar way.
However, these medicines have potential side effects. In addition, they do not do anything to help your body build stronger bones. They slow down the rate of loss but leave you with brittle fragile bones.
That’s why here at GLOW Natural Wellness, we do not recommend any osteoporosis medications as those do nothing to improve bone density. Luckily there are natural ways to boost your bone health as you transition into menopause.
Natural Ways to Boost Your Bone Health During Menopause

It’s not a secret that menopause can wreak havoc on your bones. But it’s a secret that you don’t have to let it.
Bone health is an important issue for women at any age, but it’s especially important during menopause because as estrogen levels decline, so does calcium absorption in the body. In fact, by age 30, you have achieved your peak bone mass.
After that, your body begins to lose bone—and the loss becomes more rapid as you approach menopause. In fact, bone loss 2 to 3 years before and after menopause is faster than at any other time in a woman’s life.
So, how do you keep your bones strong while going through menopause?
The key is maintaining estrogen levels as you age. This will help prevent bone loss and keep your body strong—even during menopause. This can be done safely through topical, bioidentical hormone replacement. (Click Here to Watch my FREE Masterclass where I share the myths and truths about hormone replacement and how you can access plant-based natural hormone replacement safely and affordably.)
There are natural ways you can help maintain your estrogen levels during menopause and help boost bone health. Here are our top 6 natural ways to boost your bone health during menopause:
1. Eat Right
Eat foods rich in phytoestrogens. Phytoestrogens are plant-based compounds that act like estrogens in the body. They can help combat osteoporosis by increasing bone mineral density and reducing bone loss. Foods like legumes, flaxseed, and some nuts contain high amounts of phytoestrogens; however, be sure to limit your consumption of soy products since they may have adverse effects on the thyroid gland.
Another is by eating plenty of food rich in calcium and Vitamin D. Calcium-rich foods include dairy products and leafy greens. Calcium is an important nutrient for strong bones because it helps build new bone tissue. A diet rich in calcium helps prevent bone loss and fractures by supporting healthy cell growth and development. Try adding things like spinach, almonds, kale, and broccoli into your meals!
Vitamin D helps your body absorb calcium from food sources and supplements, which is essential for building strong bones. Make sure you’re getting enough by eating fatty fish like salmon and tuna; eggs; and cheese—or taking a supplement if necessary.

Estrogen production is dependent on the proper balance of nutrients in your diet. In particular, calcium and vitamin D are crucial to maintaining healthy bones. If you don’t get enough of these nutrients from food, consider taking a supplement to ensure that you’re getting enough.
2. Improve Your Gut Health
One important way to maintain estrogen levels is to improve your gut health. This can help prevent the loss of nutrients that contribute to bone health. The gut is where the body breaks down nutrients and absorbs them into the bloodstream. When you have a healthy digestive system, you can absorb more nutrients from what you eat and keep your estrogen level high—which means stronger bones and less risk of osteoporosis.
How do you improve your gut health? You can start with something as simple as eating more fiber-rich foods like fruits, vegetables, beans, legumes, nuts, and seeds. You can also try taking a probiotic supplement (like my favorite, Megasporebiotic) once per day to help balance out your gut bacteria and make sure that there are enough good bacteria in there for your body to work properly.
Be sure to eat a diet rich in whole grains, fruits, vegetables, nuts, seeds, legumes, and fish—all foods that have high levels of vitamins D and K2. These vitamins are essential for keeping calcium in your bones where it belongs!
3. Get Moving!
Another way to ensure proper estrogen balance is by getting enough exercise every day. Physical activity helps reduce stress levels which lower cortisol production and affects hormones negatively including estrogen.
An active lifestyle will strengthen your muscles and bones. Exercise is a great way to burn calories and release endorphins—both of which help improve mood and reduce stress levels—but it also increases blood flow to your muscles and bones, which helps keep them strong.

Regular exercise also increases your metabolism, which helps to burn fat more efficiently and increase muscle mass. Exercise is one of the best ways to boost bone density—and it doesn’t have to be strenuous! Try taking walks around the neighborhood or participating in bone builder strength classes at the gym. (Tip: Most gyms around the country offer free classes to seniors through a program called Silver Sneakers)
Studies have shown that weight-bearing exercises like walking, running, and lifting weights can help increase bone density over time and reduce your risk of osteoporosis later in life.
Weight-bearing exercises include walking, jogging, running, dancing (if done regularly), hiking, and climbing stairs. These are weight-bearing exercises since they require weight on the legs/feet while performing these activities. This helps build muscle mass and strength throughout the body including muscles responsible for supporting bones such as thigh muscles.
4. Get Enough Sleep Every Night
Studies show that getting enough sleep helps regulate hormones naturally so they produce enough estrogen for healthy bones during menopause or any other time you might be experiencing low levels due to stress or illness.
5. Take Supplements

In addition to exercise and a healthy diet, research suggests that some supplements may also help to improve bone health. Calcium, Vitamin D, magnesium, and Vitamin K are important nutrients for bone health.
You may also want to consider taking a calcium supplement every day if you aren’t getting enough from your diet or if you’re at risk for osteoporosis due to low levels of estrogen production in your body (such as after having had a hysterectomy).
6. Hormone Replacement Therapy
Possibly the best treatment option for perimenopausal and post-menopausal women involves bioidentical hormone replacement therapy (BHRT), which replaces estrogen (and progesterone) in postmenopausal women who no longer produce enough of it naturally during menopause. Hormone replacement helps build up bone mass by replacing hormones lost during menopause while reducing fracture risk in those with osteoporosis who take it regularly over time.
Consider Bioidentical Hormone Replacement Therapy (BHRT). There are natural ways to maintain estrogen levels, but if you’re looking for an alternative that’s just as effective, consider bioidentical hormone replacement therapy (BHRT).

In contrast to the traditional HRT, BHRT uses hormones identical to those produced by the body, which means they will be absorbed by your body in the same way your endogenously produced hormones are, without the potential side effects that come with synthetic hormones.
Another benefit of BHRT is it helps with other menopausal symptoms such as hot flashes and night sweats.
If you’re looking for more about the benefits of bioidentical hormones, the dangers of synthetic hormones, and whether treatment with bioidentical hormones is right for you, check out our FREE Hormone Restoration Masterclass today.
Takeaway
There’s no doubt that menopause is a difficult transition. Not only are you dealing with changes in your hormones and body, but you also have to learn how to adapt to them.
Many women find it difficult to maintain their bone health during this time because their estrogen levels are lower than they were before. This can cause bone loss and increase the risk of osteoporosis later in life, which can lead to increased fractures and chronic pain.
Fortunately, there are some things you can do that will help reduce these risks.
Protecting your bone health during menopause and beyond requires careful attention to nutrition, exercise, and lifestyle habits.
- Posted
- in Hormones
- By Dr. Michelle






72 Comments
I was taking bio-identical until about 2 or 3 months. Getting a bone density test next week. Worried about my test, how it will turn out. I am 73 now. We moved and got to expensive.
Vickie
The benefits of BHRT are compounded, so you will have benefits for the years your were on hormones. We do offer very inexpensive BHRT, telemedicine and testing through our Healthy Hormone Club BHRT program. I feel that hormones should be accessible to all women regardless of their location or financial status.
Is there an age limit for Bio identical hormones
For topical bioidentical hormones that are dosed and delivered appropriately for the individual there is no upper age limit!
I really liked your article post.Much thanks again. Want more.
Muchos Gracias for your blog.Thanks Again. Cool.
A round of applause for your article. Really Great.
I really enjoy the article. Will read on…
Thanks-a-mundo for the article.Much thanks again. Fantastic.
I appreciate you sharing this blog post.Thanks Again. Want more.
A round of applause for your blog post.Really looking forward to read more. Want more.
Very good blog article. Cool.
A round of applause for your blog article.Really looking forward to read more. Great.
Very informative blog article. Keep writing.
I really like and appreciate your blog post.Much thanks again. Really Great.
Im obliged for the post.Much thanks again. Want more.
I am so grateful for your article. Want more.
Say, you got a nice blog.Really looking forward to read more. Awesome.
Very good blog post.Really thank you! Much obliged.
wow, awesome post.Thanks Again. Will read on…
I truly appreciate this blog post. Keep writing.
I cannot thank you enough for the article.Really looking forward to read more. Want more.
Muchos Gracias for your post.Really looking forward to read more. Really Great.
Major thanks for the blog post.Really looking forward to read more. Great.
I really like and appreciate your article.Thanks Again. Fantastic.
Say, you got a nice blog. Fantastic.
I really like and appreciate your blog article.Thanks Again. Really Cool.
I loved your blog.Really looking forward to read more.
Very neat blog.Thanks Again. Really Great.
Very good article.Much thanks again. Fantastic.
Very informative blog article.Really looking forward to read more. Will read on…
wow, awesome post.Much thanks again. Much obliged.
Thanks for sharing, this is a fantastic article.Thanks Again. Cool.
Thank you for your post.Really thank you! Awesome.
Fantastic post. Will read on…
Really informative article.Thanks Again. Fantastic.
Muchos Gracias for your blog.Really looking forward to read more. Great.
Thanks again for the blog. Cool.
Very informative blog article. Much obliged.
Very good blog post. Cool.
Very neat post.Really looking forward to read more. Really Great.
I really enjoy the article post. Cool.
Thanks a lot for the blog article.Thanks Again. Fantastic.
I cannot thank you enough for the blog article. Awesome.
Major thanks for the blog article.Really looking forward to read more. Awesome.
I loved your blog.Thanks Again. Want more.
A round of applause for your article post.Really looking forward to read more. Much obliged.
Looking forward to reading more. Great article.Much thanks again. Keep writing.
Say, you got a nice article post.Thanks Again. Will read on…
Say, you got a nice article.Much thanks again. Want more.
Im thankful for the blog.Really thank you! Much obliged.
I truly appreciate this blog post.Much thanks again. Fantastic.
Major thankies for the blog article.Really thank you! Awesome.
I value the article post.Really thank you! Really Great.
I cannot thank you enough for the post.Really looking forward to read more. Cool.
Great post.Thanks Again. Fantastic.
Enjoyed every bit of your blog post.Much thanks again. Want more.
Thank you for your article.Thanks Again. Cool.
I really liked your article.Much thanks again. Will read on…
Thank you for your post.Thanks Again. Really Great.
I think this is a real great article. Much obliged.
Hey, thanks for the post.Thanks Again. Awesome.
Thank you for your article.
Very neat blog post. Fantastic.
Great, thanks for sharing this post.Thanks Again.
Hey, thanks for the blog.Really thank you!
Im grateful for the article post.Really looking forward to read more. Cool.
wow, awesome article.Thanks Again.
Very neat blog.Much thanks again. Will read on…
wow, awesome blog article.Really looking forward to read more. Great.
Major thankies for the blog.Thanks Again. Much obliged.
I appreciate you sharing this article.Really thank you! Really Cool.